NURSES showed off ways to minimise the risk of pressure ulcers.
The sores can cause terrible pain and, if left untreated, rot away into weeping open wounds.
Ensuring that the ulcers don’t develop in the first place is essential, say the Great Western Hospital’s community nurses.
Experienced health workers met at the GWH’s Orbital Shopping Park base, hoping to pass on tips to care workers, student nurses and others.
They spent the morning showing off state-of-the art kit to help slash the risk of ulcers developing. They included a retro air mattress, designed to minimise the pressure on any one part of the body. A nutritionist was on hand to advise on diet – another factor in making sure that skin remains healthy.
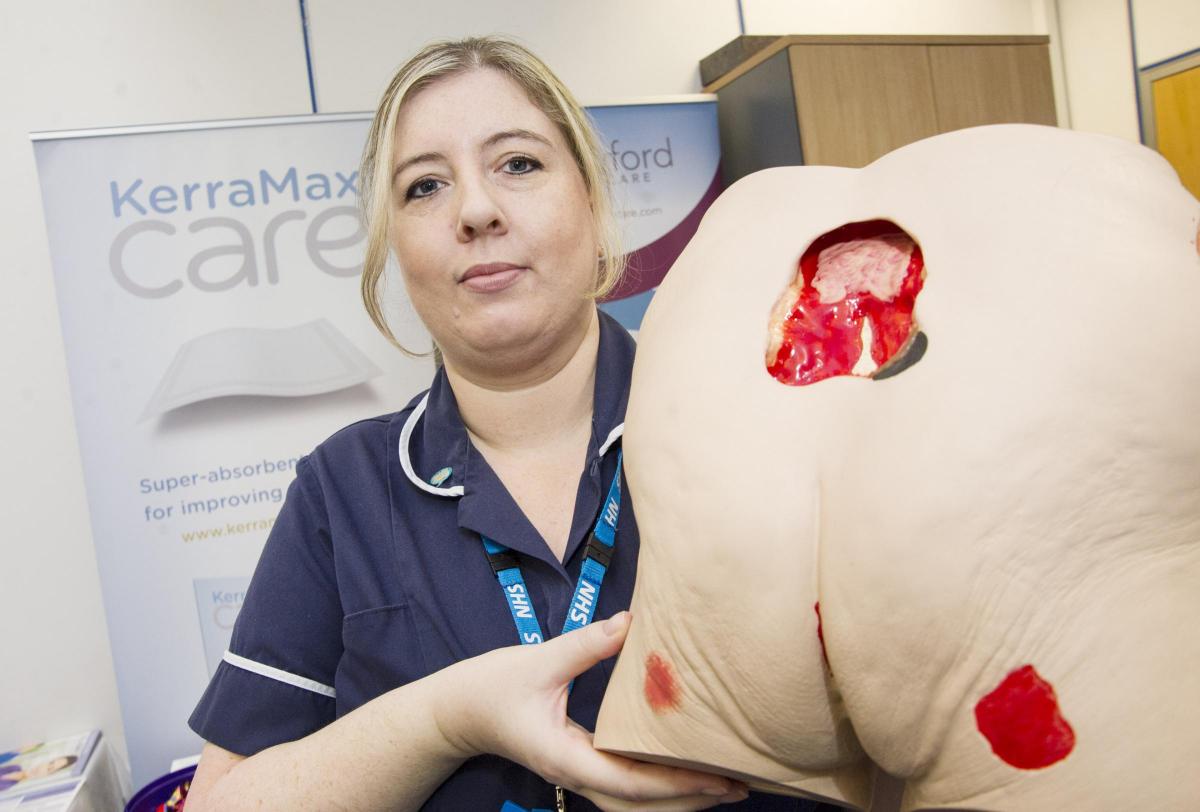
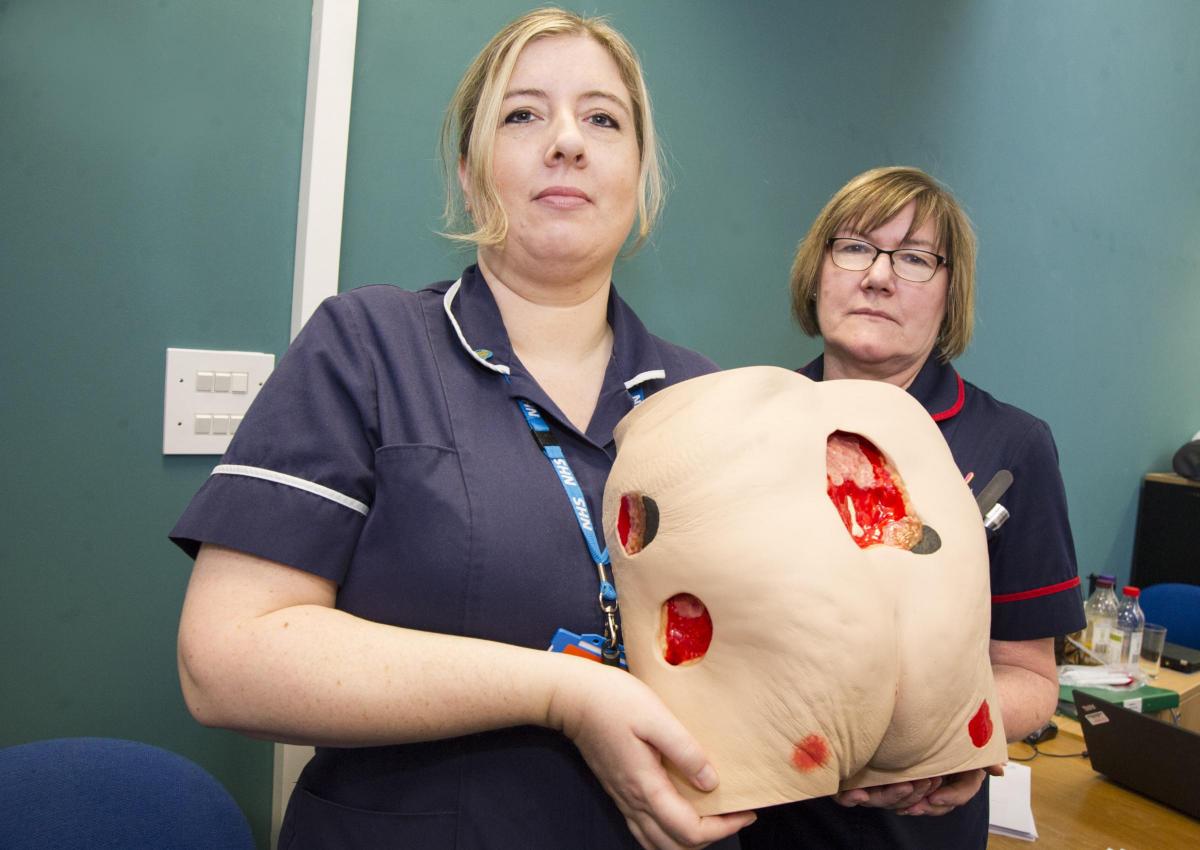
Organiser Laura Deville, a tissue viability nurse for Great Western Hospitals NHS Foundation Trust, said: “Today is really about recognising that pressure ulcers are an issue – and to promote prevention.”
She said that staff from care homes and nursing homes had been invited to the event. “We have lots and lots of nursing students here too, which is great,” she added.
Great Western Hospital has seen a drop of 60 per cent since 2015 in the number of pressure ulcers developing on the wards.
The trust has the lowest pressure ulcer rate in the South West, with around five in every 15,000 patients expected to develop a sore.
All inpatients are now given a skin assessment within two hours of being admitted to hospital.
Despite the success GWH’s community nurses want to ensure that that success is replicated away from the wards.
Laura said: “There’s always room for improvement.”
She said that all the GWH’s occupational therapists and physiotherapists were now treated to look for the signs of developing pressure ulcers, which might start as redness on the skin.
The injuries could affect anyone who spends periods of time immobile, she said. Things like incontinence or poor diet can increase the risk, as it reduces the skins natural ability to recover.
Laura added: “If you feel you know or look after somebody like that there’s no harm in approaching your local nursing service or GP.”
Colleague Nathalie Haddrell, a tissue viability nurse, added: “If you can stop a pressure ulcer from developing, you can save the patient a lot of pain and the NHS thousands of pounds.”
Nurse Laura said that her team tried to take a holistic approach to managing wounds. “We deal with the wound, but we treat the person as well.
“You should ever underestimate the profound affect having a wound has on somebody.”





Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules here